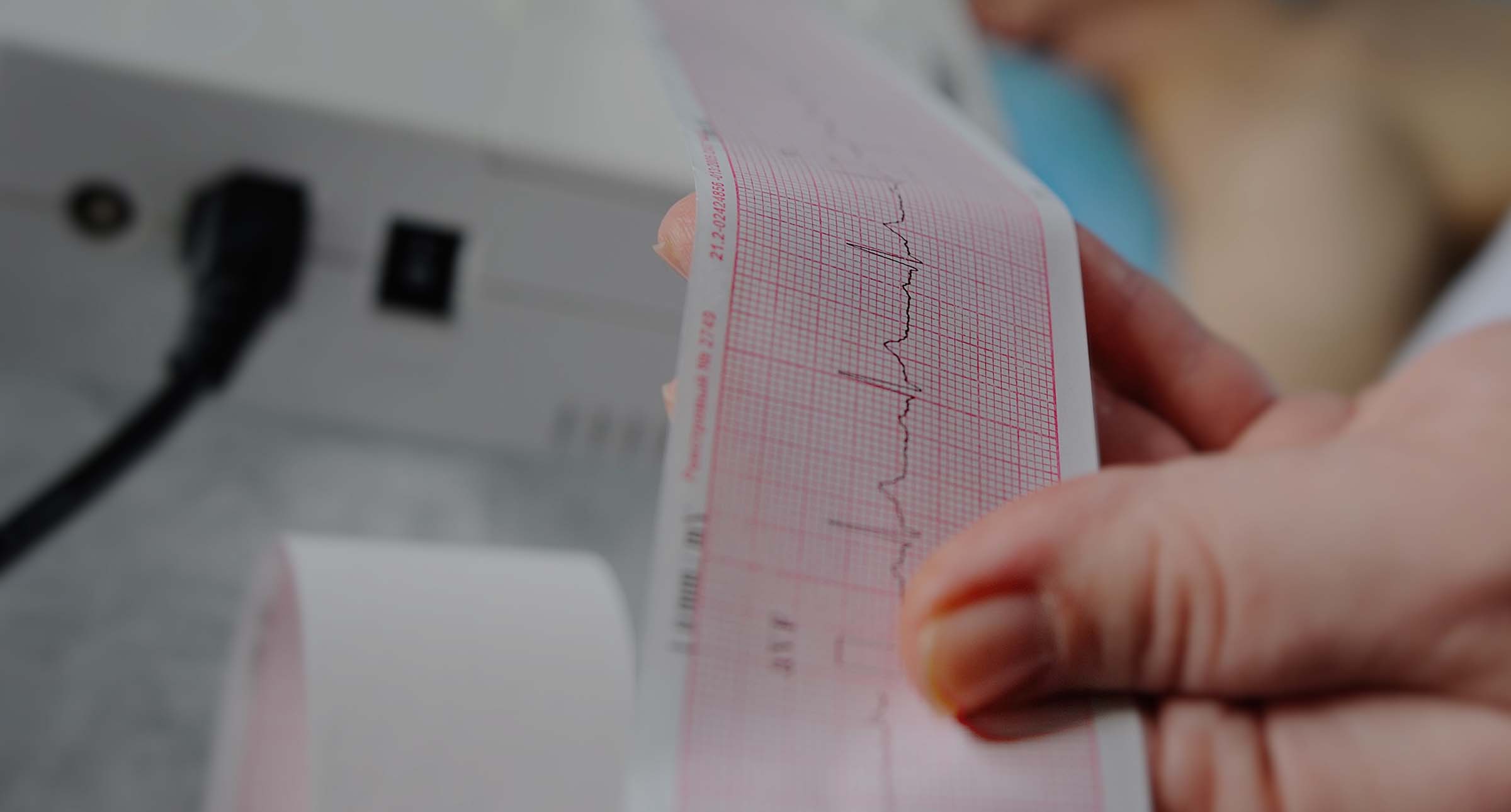
Paediatric cardiac surgery on the brain

I recently revisited an investigation of 2010 into standards of paediatric cardiac surgery at Oxford, in the context of an ongoing case. Briefly, the facts of this were as follows: paediatric cardiac surgery was suspended in March 2010 following the occurrence of four infant deaths within a 30-day period. No direct errors of judgment were found, but supervision and surgical management at the unit were found to be poor and there was what was described as a “closed culture”. The incident was reported in various publications including the British Medical Journal (BMJ). Following the investigation the paediatric cardiac unit, which was already the smallest one in England, closed.
What is now less well remembered is that there was a previous investigation into the same paediatric cardiac unit in 2000 (see this article from The Guardian) which branded the unit as “chaotic” and suggested that one senior member of the surgical team had “tended to isolate himself from others in the unit”, and wished to build up his own research team.
The findings of the two reports are worryingly similar and if you put them together (which generally the press in 2010 didn’t), tend to suggest that there may have been a period of years during which the unit may not have been as well run as it could have been – and by extension during which it wasn’t paying as much attention as it might have done to the 2001 findings.
Interestingly, the available mortality statistics, which paediatric cardiac units have been obliged to report centrally following on from the Bristol Royal Infirmary paediatric cardiac scandal, do not identify Oxford as an outlier. On the face of it this is reassuring. However, mortality statistics don’t tell you the whole story, because they don’t identify other adverse outcomes. In paediatric cardiac surgery adverse outcomes can include:
- adverse cardiac outcomes (e.g. where the heart functions poorly, potentially causing the patient to remain functionally impaired and/or in need of more treatment);
- brain damage, including but not limited to strokes;
- damage to other organs;
- late mortality (i.e. premature death, which occurs outside of the timeframes during which mortality is customarily measured for reporting purposes).
It has been well established since the 1990s that for every surgical death, there are likely to be “near misses” (Samer et al, 2003) preceding it: if these are not highlighted for investigation, death can be the last chance saloon for identifying underlying surgical issues. In themselves, near misses can have consequences, and brain damage is a particular concern. In paediatric cardiac surgery, brain damage can occur via a considerable number of routes. These are three of the main ones:
- extended time on cardiopulmonary bypass (CPB – when the body’s circulation of blood is handled by an external machine). Bypass is not a perfect analogue for the heart, and can create issues – very small impurities (“microemboli”) are particularly worrisome, and over time these accumulate. These materials then sit in the circulation and if there is a build up over time, problems can occur – the longer the patient spends on bypass, the more likely these potential issues are to eventuate;
- similarly, CPB does not replicate the action of the heart, which means that over time, organs supplied with blood from it may suffer because they are only receiving an analogue of normal circulation. This carries the risk of often diffuse but significant damage to all organs, but particularly the brain (which is particularly reliant upon oxygenated blood). Damage of this sort can be focal (affecting a particular part of the brain) or global (diffuse widespread damage). Such injuries can manifest in many ways, including behavioural and cognitive issues, difficulties with movement and potentially loss of sight (cortical blindness);
- thirdly, if the heart is not de-aired thoroughly before it starts pumping again after the procedure, then there is a risk that bubbles of air will be pushed into the arterial circulation. Once there, they will preferentially lodge in the coronary arteries (causing a heart attack) or cerebral vasculature (causing strokes). Children’s brains are more plastic than adult brains, but even so, a stroke is a stroke – and can be devastating.
At Oxford and elsewhere, brain injuries are a known risk in cardiac surgery. These risks are universal, but (like much else in surgery) can be managed, and mitigated. In a chaotic unit, management is inherently more likely to be difficult: if people aren’t speaking to each other, they won’t function optimally as a team.
Based on years of experience running cases involving brain injuries stemming from heart surgery at the Bristol Royal Infirmary, my suspicion is that the repercussions of what was identified in the reports extend beyond the deaths that prompted the 2010 report, and that similar issues at other units may well be waiting to be discovered.
Contact Joachim.
Related services & support.
More insights from our expert team.
View more articles related to Cardiac negligence and Medical negligence