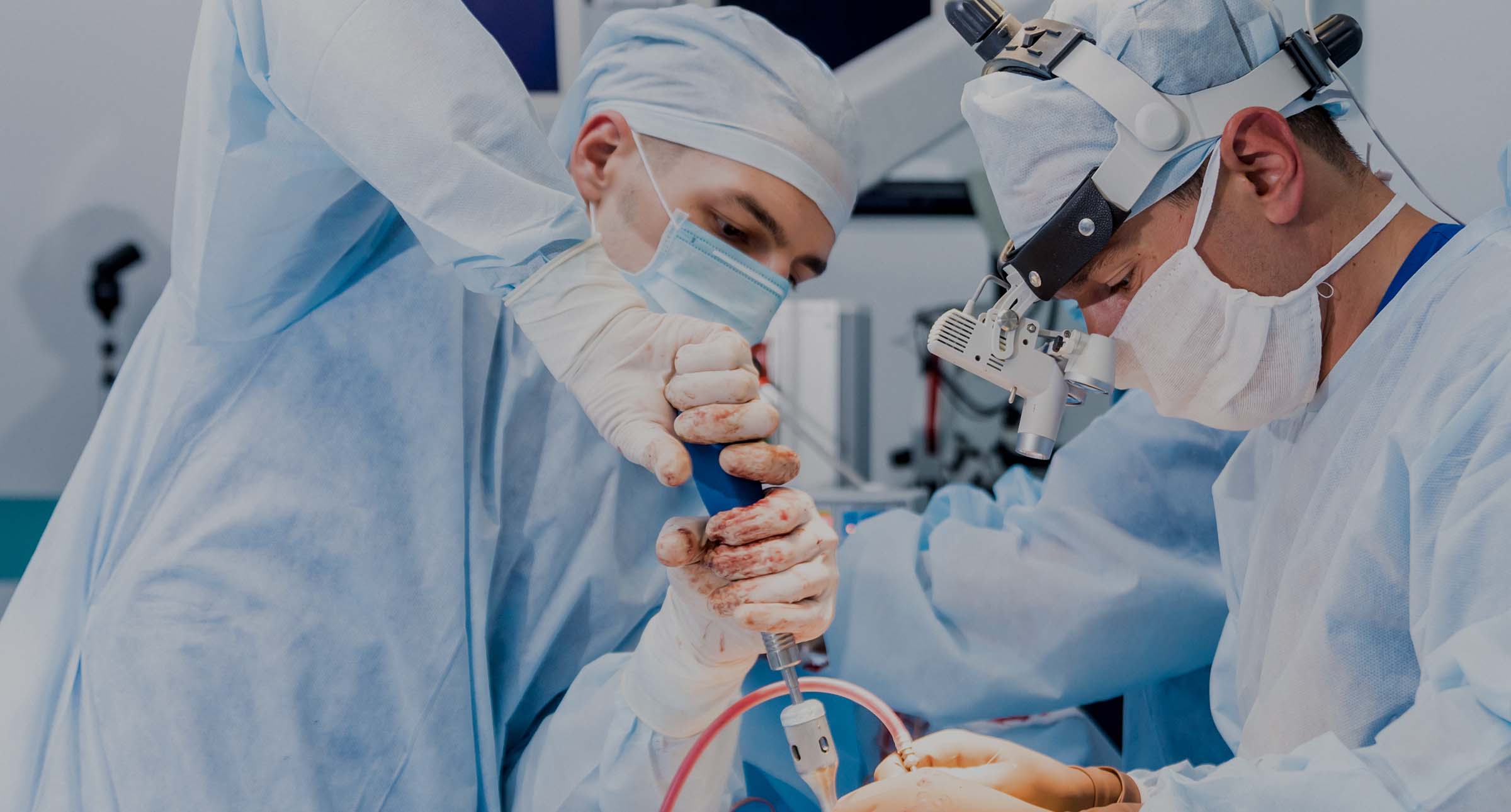
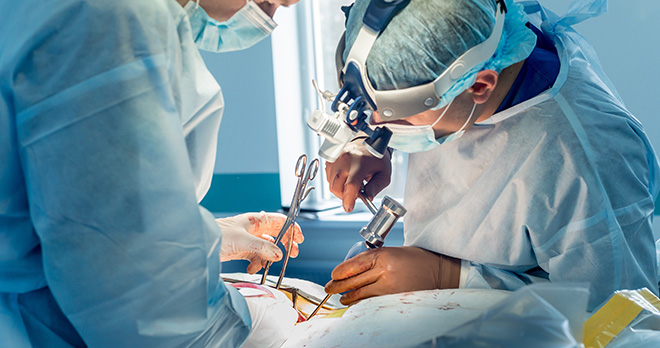
Paralysis following spinal surgery – what happens when spinal cord monitoring during surgery isn’t managed properly?
If you or someone close to you has undergone (or is soon to be undergoing) spinal surgery, you will likely be aware of the level of risk. However, surgeons have ways to mitigate this risk.
Here’s what you need to know about what should be done to monitor you, and what might have happened when something’s gone wrong in spinal surgery.
What precautions should be taken during spine surgery?
Spinal surgery is by definition dangerous, because it takes place in proximity to the spine and the spinal cord.
Damage to the spinal cord can lead to death or paralysis. In addition, damage to any of the nerves in proximity to the spine can have disastrous long-term consequences in terms of pain and function.
Certain types of spinal surgery, such as scoliosis correction surgery, carry particular risk as they involve straightening the spine with rods, which can cause pressure to the spinal cord. It is vital to monitor spinal cord function during such procedures, as an early warning system can enable the procedure to be appropriately adjusted or, if necessary, stopped before permanent damage is done.
What complications of spinal surgery should be monitored for during surgery?
Injury to the spinal cord can occur as a result of a variety of mechanisms during spinal surgery. These include:
– ischaemic injury due to a systemic problem with oxygen delivery;
– ischaemic injury due to focal vascular compromise;
– a direct traumatic/contusional injury to the cord; or
– some combination of the above factors.
It is essential to monitor spinal cord function, as any injury to the spinal cord, whether ischaemic or traumatic, will be detectable with appropriate monitoring.
What type of monitoring is required in neurosurgery involving the spine?
Electrical stimulation to nerves and muscles in the body, while recording a response to such electrical stimulation in the brain, can measure the level of spinal cord function which is transmitting the electrical signals. This gives an early warning sign of any damage to the spinal cord.
What are the methods of neuromonitoring?
There are two types of neuromonitoring, Somatosensory Evoked Potentials (SSEPs), and Trans-cranial Electrically Stimulated Motor Evoked Potentials (TcMEPs).
-
SSEPs
Somatosensory Evoked Potentials (SSEPs) are obtained by administering an electrical stimulus in an upper or lower limb nerve. The response will then be recorded on the scalp overlying the region of the brain responsible for a particular type of sensation (the somatosensory cortex). The time taken for the impulse to reach the brain (latency) is established as a baseline at the beginning of the procedure, and the size (amplitude) of the response is calculated, and again used as a baseline.
SSEPs are then measured almost continually during a spinal procedure, and a significant increase in latency or a significant decrease in amplitude can indicate deteriorating spinal cord function. The SSEPs enable the surgeon to be alerted to deteriorating function and make necessary changes in the surgical procedure to try to prevent permanent neurological injury.
-
TcMEPs
Trans-cranial Electrically Stimulated Motor Evoked Potentials (TcMEPs) are performed by stimulating the scalp overlying the part of the brain required to perform movement (the primary motor cortex). An electrical stimulus is generated from the primary motor cortex which passes down the anterior spinal cord and ultimately reaches the muscles in the head, neck, arms, torso and legs. Appropriate muscles can be selected to measure the size of responses produced in the muscles, and again this can be used as a baseline measure of anterior spinal cord function.
Do SSEPs and TcMEPS have different functions?
Although they broadly serve the same function, there are some important differences. The somatosensory fibres relating to the generation of the SSEP are found in the posterior (back) part of the spinal cord, in the dorsal columns. The posterior spinal cord has a different blood supply to the anterior (front) cord, therefore it is possible to have intact dorsal columns but significant injury to the anterior spinal structures. As a consequence, SSEPs alone do not adequately monitor function in the anterior spinal cord.
SSEPs and TcMEPs are used together in the course of spinal surgery with the aim of monitoring the anterior and posterior spinal cord. The use of only one method of monitoring risks a surgeon missing evolving pathology in the part of the spinal cord not being monitored.
What are evoked potentials in spinal surgery?
Electrical stimulation to nerves and muscles in the body, while recording a response to such electrical stimulation in the brain, can measure the level of spinal cord function which is transmitting the electrical signals. The level of response recorded gives an early warning sign of any damage to the spinal cord.
There are two types of neuromonitoring, Somatosensory Evoked Potentials (SSEPs), and Trans-cranial Electrically Stimulated Motor Evoked Potentials (TcMEPs) covered in further detail above.
What is the wake-up test for spinal surgery?
Before intraoperative neurophysiological monitoring became widely used, the wake-up test was the only test for spinal cord integrity during spinal surgery, and in particular surgery to correct spinal deformity. It remains a useful test for resolving uncertainty in intraoperative monitoring, or if intraoperative monitoring fails or becomes unavailable.
The patient is awakened during surgery, after the main part of the surgery has been completed (e.g. after placement of the rods in spinal deformity correction surgery). The patient remains on the table and intubated with the surgical site still open, whilst anaesthetic is discontinued or significantly lightened. Neuromuscular blockade needs to be avoided when performing the wake-up test, as this would impair the patient’s ability to move their limbs.
Once the patient is sufficiently awake, they are asked to move their feet. If they are able to do so, this demonstrates intact spinal cord motor function. When the test is complete, anaesthesia is reinstituted, the surgical procedure is completed, and the back is closed.
The usefulness of the wake-up test is now a matter of controversy. Some consider it to be entirely obsolete, but others take the view that it can have its place in certain circumstances, where intraoperative monitoring fails or is unavailable.
What are the benefits of intraoperative monitoring?
There are significant benefits to intraoperative monitoring for patients undergoing spinal surgery which may threaten the integrity of the spinal cord. In such procedures, which include scoliosis correction surgery, it is essential to monitor spinal cord function during the surgery, as the monitoring can provide an early warning signal of damage to the spinal cord, so that the surgery can, if necessary, be stopped to prevent further damage.
When is paralysis as a result of monitoring failure a result of negligence?
Now that intraoperative neurophysiological monitoring is routinely available in the form of Motor Evoked Potentials (MEPs) and Somatosensory Evoked Potentials (SSEPs), it would usually amount to sub-standard surgical care to proceed with any surgery which threatens the integrity of the spinal cord without using such monitoring.
If a patient were to be paralysed during spinal surgery (and in particular surgery to correct spinal deformity) and intraoperative neurophysiological monitoring was either not utilised, or was not working satisfactorily during the operation, then there could well be a finding of negligence against the surgical team (including the neurophysiologist responsible for interpreting the evoked potentials).
RWK Goodman has successfully recovered millions of pounds of compensation for patients paralysed as a result of the negligent failure to utilise appropriate intraoperative monitoring during surgery to correct spinal deformity.
Is intraoperative neuromonitoring a standard of care?
During spinal surgery which threatens the integrity of the spinal cord, there is a duty of care upon the surgical team to protect the spinal cord.
The appropriate standard of care in spinal surgery (and in particular in surgery to correct spinal deformity) is always to utilise intraoperative neurophysiological monitoring. Failure to do so is likely to be seen by a court as sub-standard care amounting to negligence.
If you are living with paralysis or another injury as a result of spinal surgery, and think your treatment may have been negligent, our spinal surgery solicitors are here to help.
Call now